What is IBS?
Irritable bowel syndrome (IBS) is a functional gastrointestinal conditon involving the gut-brain axis that affects the large colon or bowel, and it is characterised by abdominal pain, discomfort, and changes in bowel habits (constipation, diarrhoea or both). IBS affects 3.5% Australians and 5-10% of people worldwide and there are three main subtypes:
- IBS C: constipation predominant
- IBS D: diarrhoea predominant
- IBS M: mixed pattern
Common Symptoms of IBS
Symptoms can vary between individuals but may include:
-
- Abdominal pain or discomfort
- Bloating and distension
- Gas and flatulence
- Urgency to pass a bowel motion
- Changes in stool form or frequency
- Fatigue related to digestive discomfort
When to Seek Medical Advice
It is important that IBS is properly diagnosed by a health professional to rule out other conditions such as:
- Coeliac disease
- Inflammatory bowel disease
- Endometriosis
- Gastrointestinal infections
Red flags that might need investigation
- Being over 40 and a family history of bowel cancer or inflammatory bowel disease
- Unintentional weight loss
- Blood in stools
- Recent change in bowel habits when over 50 years
- Iron deficiency anaemia on blood test
- Faecal occult blood test result is positive
- Bowel motions at night
What Can Trigger IBS Symptoms?
The exact cause of IBS is not fully understood, however common contributing factors include:
- Stress and psychological factors
- Dietary triggers
- Changes in gut microbiota
- Altered gut motility
- Previous gastrointestinal infections
Symptoms may also develop following antibiotic use or periods of high stress.
Common Food Triggers
Certain foods and drinks can trigger IBS in some individuals:
- Lactose (milk sugar) containing foods (milk, some yoghurts, ice-cream)
- Alcohol
- Gas forming foods such as onion, garlic, brussel sprouts, cabbage, cauliflower, dried beans and lentils
- Artificial sweeteners (sorbitol, mannitol, aspartame)
- Caffeine
- Gluten- hypersensitivity can mimic IBS
Identifying individual triggers can be helpful as tolerance varies.
Evidence Based Approaches to Managing IBS Symptoms
There are a range of treatment options for IBS, although not all of them are specific to treating IBS and may be more targeted at managing the symptoms. Therefore management strategies are typically individualised and may involve a combination of dietary and lifestyle approaches.
1. Dietary Approaches
A low FODMAP diet has been widely studied and may help reduce symptoms in some individuals. This approach involves temporarily reducing certain fermentable carbohydrates, followed by structured reintroduction.
This should ideally be done under guidance from a qualified health professional.
2. Fibre Intake
Different types of fibre can have different effects:
- Soluble fibre such as psyllium may be better tolerated
- Insoluble fibre such as wheat bran may worsen symptoms in some people
3. Probiotics and Gut Microbiota
There is growing research interest in the role of the gut microbiome in IBS.
Some studies have investigated specific probiotic strains, in relation to digestive symptoms. However, outcomes can vary depending on the strain, dose and individual response. Sometimes probiotics in general can be useful for supporting symptoms such as gastrointestinal pain or reducing flatulence.
4. Lifestyle Strategies
Lifestyle factors can play an important role in symptom management:
- Eating smaller, regular meals
- Reducing intake of trigger foods
- Managing stress
- Gentle physical activity
Practices such as yoga and relaxation techniques may also support overall wellbeing and gut function.
5. Stress and the Gut Brain Axis
The gut and brain are closely connected. Stress and anxiety can influence gut sensitivity and motility.
Approaches such as gut directed hypnotherapy and mindfulness based strategies are areas of ongoing research interest.
What is low FODMAPS Diet?
FODMAPs are types of carbohydrates that are poorly absorbed in the small intestine and can be fermented by gut bacteria.
This process may lead to:
- Gas production
- Increased water in the bowel
- Bloating and discomfort
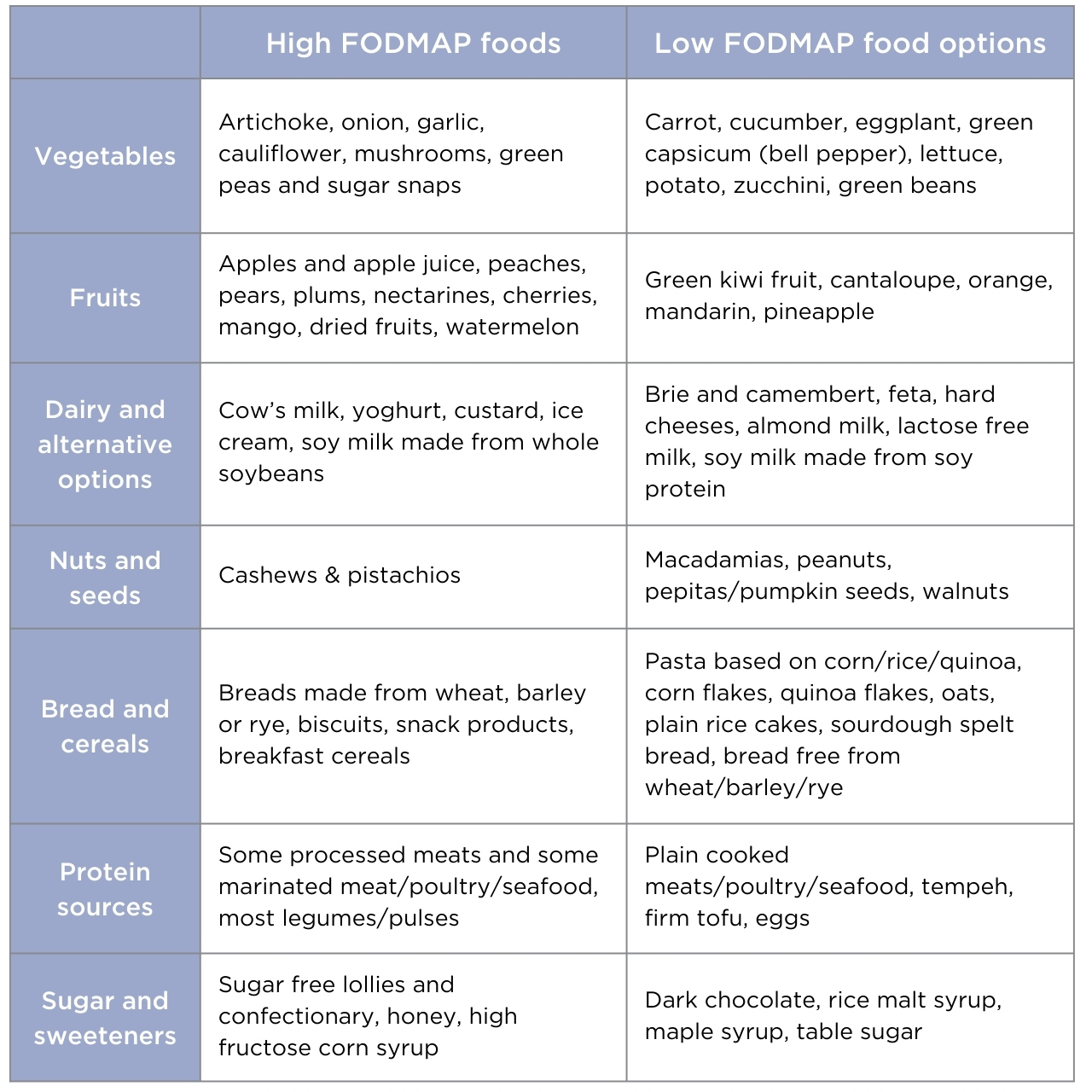
Researchers at Monash University in Victoria, Australia were the first to discover the low FODMAPS diet and to research which foods are high in FODMAPS and low in FODMAPS (See Table 1).
Table 1. High and low FODMAP FOODS adapted from Monash University.
Who Should Follow a FODMAPS diet?
Only people who are medically diagnosed with IBS should do a low FODMAP diet. A low FODMAP diet is not intended as a long term diet for the general population.
It is typically used:
- Short term (2 to 6 weeks)
- Under professional guidance
- As part of a structured reintroduction process
Key Takeaways
- IBS is a common functional gut condition involving the gut brain axis
- Symptoms and triggers vary between individuals
- Dietary and lifestyle strategies may help manage symptoms
- The gut microbiome is an area of growing research interest
- Professional guidance is important for diagnosis and management
This information is general in nature and is not intended to diagnose, treat, cure or prevent any disease. Always consult a qualified health professional for personalised advice.
Reference list
- Lacy BE et al. Bowel Disorders. Gastroenterology. 2016.
- Ford AC et al. Effect of fibre, antispasmodics and peppermint oil in IBS. BMJ. 2008.
- Halmos EP et al. A diet low in FODMAPs reduces symptoms of IBS. Gastroenterology. 2014.
- Staudacher HM et al. Mechanisms and efficacy of dietary FODMAP restriction in IBS. Gut. 2017.
- National Institute for Health and Care Excellence NICE IBS Guidelines CG61.
- Hill C et al. The International Scientific Association for Probiotics and Prebiotics consensus statement. Nat Rev Gastroenterol Hepatol. 2014.
- Ducrotté P et al. Clinical trial of Lactobacillus plantarum 299v in IBS. World J Gastroenterol. 2012.
- Monash University Low FODMAP Diet resources.





